Sacroiliac joint (SIJ) fusion can relieve pain in carefully selected cases with diagnostic confirmation after conservative treatments have failed. In 2024–2025 the evidence is mixed: there are trials favoring surgery over non-operative care, but a sham-controlled trial found no superiority at 6 months. The keys are rigorous selection (pain confirmed by diagnostic blocks, concordant clinical tests, and exclusion of other sources) and realistic expectations about benefits and risks.
- Useful for refractory chronic sacroiliac pain with a confirmed diagnosis.
- Before surgery: education, active physiotherapy, judicious analgesics, and targeted injections.
- Typical benefit: reduced pain and improved function in well-selected patients; outcomes vary by technique.
- Risks: malposition, neural/vascular injury, lack of fusion, and need for revision.
- Typical recovery: early walking; return to desk work in 2–6 weeks and heavier activity in 8–12 weeks if uncomplicated.
What is sacroiliac joint pain?
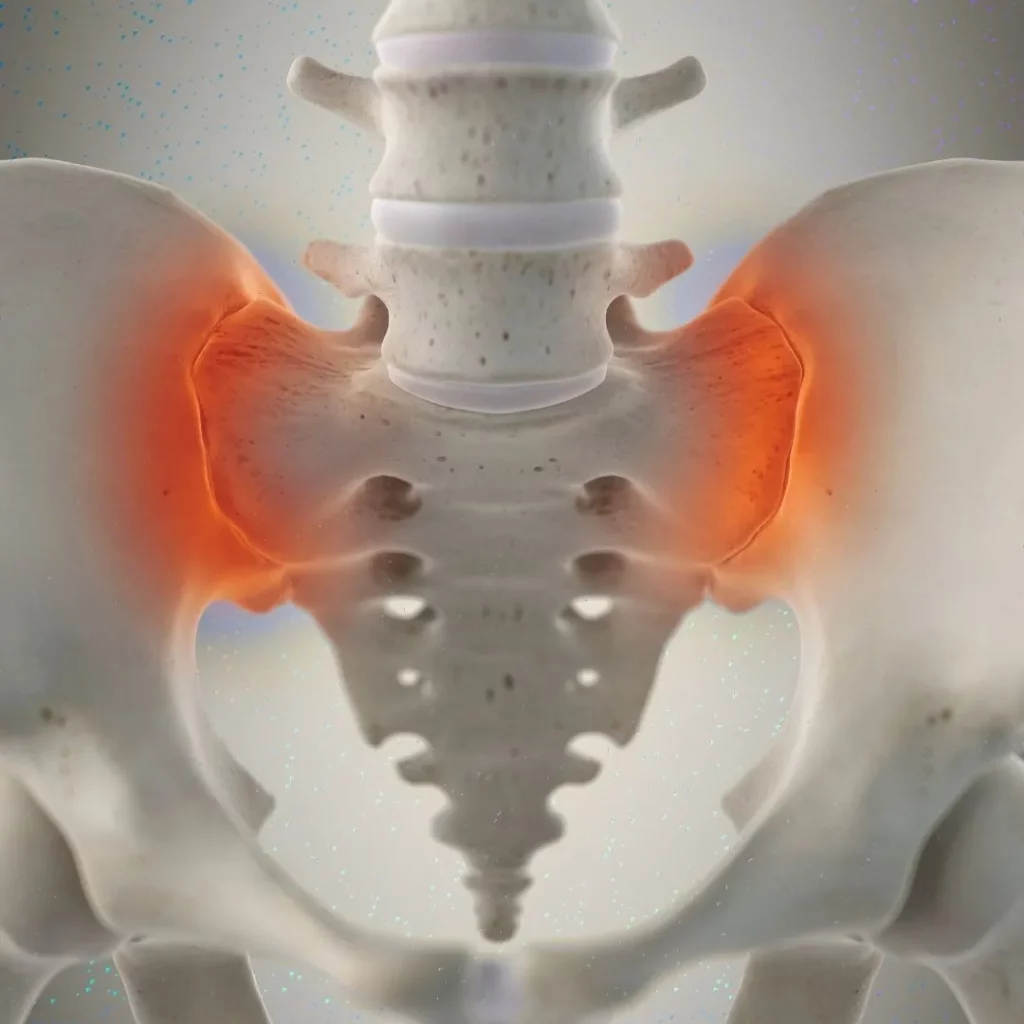
The SIJ connects the sacrum to the iliac bones. It moves only slightly, but degeneration, overload, pregnancy, trauma, or prior surgery can inflame it and cause pain in the lower buttock and lumbosacral region, sometimes radiating to the groin or the back of the thigh. Diagnosis is clinical and functional: a compatible history, positive provocative maneuvers, and—most importantly—relief after image-guided diagnostic blocks with local anesthetic.
Symptoms and indications: who might benefit?
- Pain focused in the lower buttock, worse when standing or on stairs.
- Positive clinical test cluster (e.g., FABER/Patrick, pelvic compression and distraction) performed by trained professionals.
- Confirmation with one or two diagnostic blocks of the SIJ providing significant pain relief for hours.
- Failure of a well-executed conservative plan (education, therapeutic exercise, load modification, prudent analgesics, injections) over several weeks.
- Exclusion of other main causes (severe central stenosis, dominant radiculopathy, hip pathology) on evaluation.
Tests and diagnosis that help
What usually adds value: targeted history and exam; pelvic X-rays to rule out other causes; MRI or CT if bone injury is suspected or for implant planning; image-guided diagnostic blocks that confirm the pain source. What rarely changes decisions: indiscriminate tests without clinical correlation, or injections without clear indication.
Alternatives to surgery (and when to exhaust them)
- Active physiotherapy program focused on lumbopelvic control, gluteal strength, and stabilization.
- Analgesics non-opioid, with adjuvants for neuropathic features; avoid chronic opioids.
- Injections intra-articular or periarticular with anesthetic/corticosteroid: temporary relief that also aids diagnosis.
- Radiofrequency ablation of lateral branches in selected cases.
These options should be attempted and documented before considering fusion, unless contraindicated.
What does minimally invasive sacroiliac fusion involve?
The goal is to stabilize the SIJ to reduce painful micromotion. Through small incisions, implants (e.g., screws or triangular devices) are placed from the ilium into the sacrum under X-ray or navigation guidance. Lateral and posterior/posterolateral approaches exist; they differ in trajectory, fixation, and complication profile. Surgery usually lasts 30–90 minutes per side and allows early assisted walking.
Expected benefits (and their variability)
- In well-selected cohorts, most patients report clinically meaningful improvement in pain and function within the first months.
- Trials versus conservative care have shown short-term superiority in pain/disability, but a sham-surgery trial found no differences at 6 months, underscoring the importance of selection and follow-up.
- Complication and revision rates vary by technique and experience, generally low in expert hands but not zero.
Risks and adverse effects
- Infection, bleeding, thrombosis, persistent pain.
- Implant malposition, injury to sacral roots or foramina.
- Nonunion (lack of bony fusion) and need for reoperation.
- Approach-specific issues (e.g., some series report higher complication rates with the lateral approach than with the posterior approach).
The decision should weigh pros and cons versus continuing conservative management or radiofrequency ablation.
Practical criteria for referral/surgical evaluation
- Sacroiliac pain ≥ 6 months with significant functional impact despite well-structured conservative care.
- Positive exam on multiple maneuvers and diagnostic blocks with marked relief.
- Imaging used to rule out other sources and for planning.
- Understanding of realistic expectations and commitment to postoperative rehabilitation.
Realistic recovery timelines
- Discharge: same day or next day, depending on comorbidities.
- Walking: early with aids; daily walking at home.
- Desk work: 2–6 weeks if pain is controlled.
- Physical/impact work: 8–12 weeks or more, depending on progress.
- Bone consolidation: months; clinical follow-ups and imaging when appropriate.
When to go to the emergency department
- Disproportionate pain not controlled with prescribed analgesia.
- Persistent fever, redness, or wound drainage.
- New neurological deficit (weakness, saddle anesthesia) or incontinence.
- Signs of thrombosis (swelling, severe calf pain).
Myths and realities
- “SIJ fusion always cures low back pain.” Reality: it helps only when the SIJ is the main source and this is well documented.
- “If I have surgery, I won’t need rehab.” Reality: guided exercise remains essential.
- “All techniques are the same.” Reality: approaches differ in fixation and complication profiles.
- “If I’m not better in 2 weeks, it failed.” Reality: improvement is gradual; fusion takes months.
Frequently asked questions
How is it confirmed that the pain comes from the SIJ?
With a compatible history and exam plus one or two diagnostic blocks that clearly relieve pain for hours.
Should I exhaust physiotherapy before surgery?
Yes; most people improve with an active plan and analgesic measures. Surgery is considered after documented failure.
Which technique is “better”: lateral or posterior?
It depends on anatomy and team experience. Some analyses report differing complication and revision rates between approaches.
Can both sides be operated on?
In selected cases; bilateral surgery should be individualized and may be staged.
When can I drive or return to work?
Driving once pain is controlled and you’re not taking sedatives; desk work 2–6 weeks, physical work roughly 8–12 weeks.
What if the bone doesn’t fuse?
Pain may persist and a revision may be considered; follow-up is essential to detect this early.
Glossary
- SIJ: the sacroiliac joint, between the sacrum and ilium.
- Diagnostic block: an anesthetic injection to confirm the pain source.
- Lateral/posterior approach: implant trajectory from the ilium into the sacrum via different routes.
- Nonunion (pseudoarthrosis): lack of bony consolidation after an attempt at fusion.
References
- Sacroiliac joint treatments: conservative and surgical options. https://complexspineinstitute.com/en/complex-spine-institute/en/treatments/traitements-des-articulaciones-sacro-iliaques/
- NICE. Minimally invasive sacroiliac joint fusion surgery for chronic sacroiliac pain (IPG578). 2017. https://www.nice.org.uk/guidance/ipg578
- Polly DW et al. Randomized Controlled Trial of Minimally Invasive SI Joint Fusion vs Non-Surgical Management. Neurosurgery. 2015. https://journals.lww.com/neurosurgery/fulltext/2015/11000/randomized_controlled_trial_of_minimally_invasive.2.aspx
- Randers EM et al. Minimally invasive sacroiliac joint fusion vs sham operation: double-blind RCT. EClinicalMedicine. 2024. https://pubmed.ncbi.nlm.nih.gov/38328752/
- Medani K et al. Lateral vs posterior approaches in SIJ fusion: meta-analysis. 2025. https://www.sciencedirect.com/science/article/pii/S2772529425000311
- Amer MH et al. Minimally invasive SIJ fusion: review and case series. 2022. https://pmc.ncbi.nlm.nih.gov/articles/PMC9595039/
- UnitedHealthcare Policy. Sacroiliac Joint Interventions. 2025. https://www.uhcprovider.com/content/dam/provider/docs/public/policies/index/commercial/sacroiliac-joint-interventions-12012025.pdf
Educational content. Not a substitute for individual medical evaluation or your specialist’s advice.