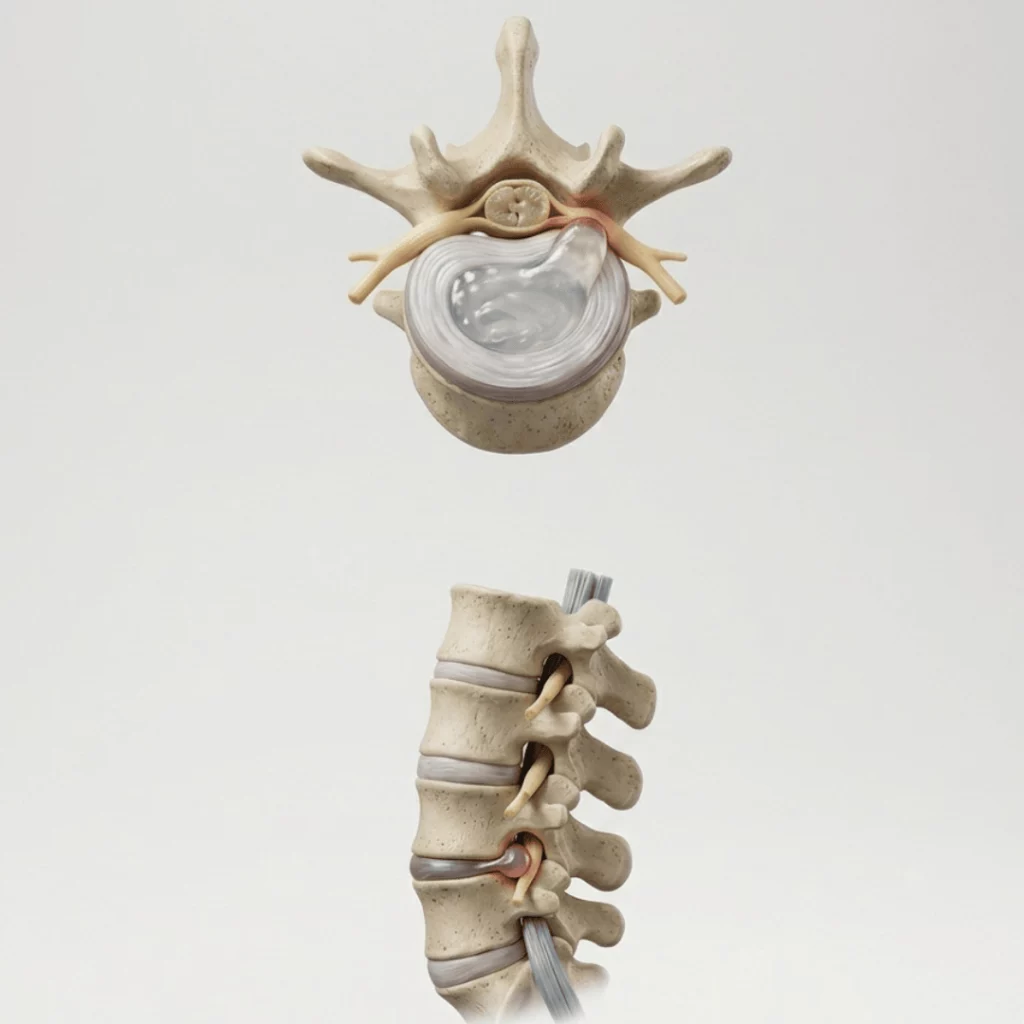
Lumbar microdiscectomy is usually considered when a herniated disc compresses a nerve root and causes persistent sciatica, disabling pain or significant neurological deficit. It is not indicated just because an MRI looks “bad.” Symptoms, examination and tests must be correlated first. In well-selected people, it often provides faster relief of radicular pain than waiting indefinitely, but it does not completely eliminate the risk of persistent pain, recurrence or the need for another surgery.
- Not every lumbar herniation requires surgery.
- Microdiscectomy is mainly aimed at leg pain from nerve compression, rather than isolated low back pain.
- MRI is very helpful, but it does not decide on its own.
- Surgery can relieve sciatica sooner when the case is well indicated.
- Recovery is usually faster than with fusion surgeries, but still requires caution and progression.
- There are real risks, such as infection, cerebrospinal fluid leak, nerve injury or recurrent herniation.
- There are emergency signs you should not wait out at home.
What is a lumbar microdiscectomy
Lumbar microdiscectomy is a surgery intended to remove, totally or partially, the disc fragment that is irritating or compressing a nerve root in the lumbar area. In simple terms, it is not about “fixing the whole back,” but about freeing the nerve that is causing sciatica.
It is called “micro” because it is performed with a more limited exposure than a classic open surgery and with the help of magnification. That usually translates into less muscle damage and a quicker recovery than more extensive operations. Even so, it remains a real surgery, with anesthesia, postoperative care and risks that must be well understood.
The clinical key is this: it usually makes more sense when the main symptom is pain that goes down the leg, with tingling, numbness or weakness, and less so when the only dominant problem is diffuse low back pain without a clear radicular component.
Symptoms and indications
The most typical situation is a person with sciatica from a lumbar herniation who has had weeks of significant leg pain, has difficulty walking, sleeping, sitting or working, and notices the problem is not improving reasonably. Sciatica is usually described as pain that travels down the buttock, thigh, calf or foot, sometimes with a feeling of electric shock, burning or current.
Among the signs that often lead to consideration of microdiscectomy are the following:
- Leg pain clearly more intense than back pain.
- Tingling or loss of sensation in a distribution compatible with a nerve root.
- Weakness in the foot or leg, for example difficulty lifting the forefoot or standing on tiptoe.
- Persistent pain despite well-performed conservative treatment.
- Clear correlation between symptoms, examination and MRI.
There are also cases in which surgery is discussed earlier. For example, when weakness progresses, when the pain is so intense that daily life is completely blocked, or when signs of severe compression appear that require urgent evaluation.
How the diagnosis is confirmed
The diagnosis should not be based solely on an image. Many people have protrusions or herniations on MRI and will never need surgery. What matters is that what is seen matches what you feel and what the clinician finds on examination.
Evaluation usually combines:
- Detailed medical history: where it hurts, where it radiates, which postures worsen or relieve it, how long it has been happening and how much it affects function.
- Neurological examination: strength, sensation, reflexes and neural tension maneuvers.
- Lumbar magnetic resonance imaging: the main test to see the disc, the root and the anatomical conflict.
- Other tests in selected cases: CT, dynamic X-rays or neurophysiological studies if there are diagnostic doubts or previous surgeries.
A common mistake is thinking that a “large” herniation forces surgery and a “small” one does not. In practice, it matters much more whether the herniation truly explains the clinical picture. A small herniation very well placed can cause a lot of sciatica, and a striking one can be almost an incidental finding.
Non-surgical alternatives
Before considering microdiscectomy, in most cases a structured conservative management is attempted. That does not mean absolute rest or resignation. On the contrary, it usually includes education, maintaining activity within tolerable limits, progressive exercise, prudent analgesia and active physiotherapy.
In some people epidural injections or selective nerve blocks are also considered, especially when they can help control a particularly painful phase or facilitate rehabilitation. They are not a definitive solution for all cases, but in selected profiles they can buy time and provide relief.
Continuing without surgery makes more sense when there is a clear trend to improvement, when strength is preserved and when functional impact begins to decrease. Waiting indefinitely stops making sense when weeks pass without progress, pain remains disabling or neurological function worsens.
Surgical alternatives
Microdiscectomy is not the only possible surgical option, although it remains a very common reference for lumbar herniation with sciatica. Depending on the case, endoscopic techniques, wider decompressions if associated stenosis exists, or fusion surgery if there is relevant instability may also be considered.
This is important because not every “lumbar hernia operation” pursues exactly the same goal. In some patients the objective is to remove a specific disc fragment. In others, it may also be necessary to widen the canal or stabilize the segment. That is why it is wise to avoid simplistic messages like “this technique is always better.” The right technique is the one that solves the real problem with the least reasonable cost.
Benefits versus risks and adverse effects
Expected benefits
The main expected benefit is relief of radicular pain, that is, leg pain. In many patients tingling, sensation and part of the weakness also improve, although neurological recovery is not always immediate or complete. The longer the nerve has been compressed and the more severe the deficit has been, the more cautious expectations should be.
Another advantage is that it usually allows a faster recovery than more extensive lumbar surgeries. Many people walk early, return home quickly and resume basic daily tasks sooner. But quick improvement does not mean full recovery in a few days. The nerve needs time to calm down and the operated tissues need to heal.
Risks and adverse effects
As with any spinal surgery, microdiscectomy has risks. Among the best known are infection, bleeding, cerebrospinal fluid leak from dural tear, nerve injury, hematoma, persistent pain and recurrence of the hernia at the same level.
It is also important to know that a technically correct surgery does not guarantee zero pain. Sometimes the nerve takes weeks or months to recover. Other times there were multiple sources of pain and decompressing one root does not eliminate all back discomfort. This does not necessarily mean the surgery was poorly indicated, but it does mean expectations should be realistic from the start.
Referral criteria
It is usually reasonable to request specialist assessment when sciatica clearly limits walking, sleep, work or autonomy and does not improve after several weeks of well-oriented conservative treatment. Referral becomes a priority when objective weakness appears, foot drop, neurological worsening or reasonable doubt about whether the problem is really a lumbar herniation or something else.
It is also advisable to speed up evaluation in people with a history of lumbar surgery, disproportionate pain, bilateral symptoms, changes in sphincter function or a clinical pattern that does not fit well with simple sciatica.
Realistic recovery times
There is no single timetable, but there are reasonable ranges. In a typical course, getting up and walking early is part of postoperative care. Basic household activities are usually resumed in a few days with caution. Sedentary work can be resumed in a few weeks if pain is controlled and breaks can be taken. Physical jobs, with lifting or repeated twisting, generally require more time and a more careful progression.
The first weeks usually focus on walking, controlling pain, avoiding overload and regaining confidence. Later, work on strength, mobility and functional tolerance is undertaken. A feeling of “tightness” or intermittent discomfort does not always mean something is wrong. What is more worrying is a clear tendency to worsen, pain that flares up again or new neurological deficits.
Factors such as smoking, obesity, diabetes, poor physical condition, high anxiety, previous chronic pain or very demanding work can lengthen recovery. It is not a matter of willpower. These are real variables that should be explained before surgery.
When to go to the emergency room
There are signs that should not be observed for days “to see if they pass.” Seek urgent medical attention if you experience loss of bladder or bowel control, numbness in the genital or perineal area, rapidly progressing weakness, high fever with intense pain, unbearable pain that does not subside or sudden neurological worsening after surgery.
Outside of these signs, many postoperative concerns can be resolved at scheduled follow-up, provided the general course is heading in a good direction.
Myths and realities
Myth: if I have surgery, my back will be like new
Reality: microdiscectomy aims to resolve a specific nerve conflict. It does not rejuvenate the whole disc nor eliminate any low back pain forever.
Myth: if I endure longer, I will almost surely avoid surgery
Reality: some people improve with time, but others plateau or worsen. The decision should not be based on enduring for the sake of enduring, but on how pain, function and strength evolve.
Myth: a large herniation always requires surgery
Reality: you treat the person, not the image. Clinical correlation matters.
Myth: after microdiscectomy I will not be able to live a normal life
Reality: many people regain very functional lives, but the process is progressive and requires reasonable habits.
Frequently asked questions
Does lumbar microdiscectomy work for any back pain?
No. Its main objective is to relieve compression of a nerve root when there is sciatica or other radicular symptoms. If the dominant problem is nonspecific low back pain without radicular correlation, the indication is very different.
How long should you wait before considering it?
It depends on the intensity of the pain, the response to conservative treatment and whether there is neurological deficit. In many cases conservative management is attempted for several weeks, but if there is progressive weakness or a neurological emergency the waiting time may be shorter.
Is recovery very painful?
It is usually more manageable than recovery from more extensive lumbar surgeries, but the first days may include discomfort in the operated area, a feeling of stiffness or residual nerve irritation.
Can I have another herniation in the same place?
Yes. Recurrence exists. It does not mean it is common in all patients, but it is a real possibility and it is worth discussing risk factors and reasonable prevention.
What if my leg pain improves but I still have some tingling?
That can happen. Pain often improves before other neurological sensations. Nerve recovery can be slower and does not always follow a linear order.
Is endoscopy better than microdiscectomy?
Not in all cases. There are situations where endoscopic surgery fits very well and others where microdiscectomy remains an excellent option. The choice depends on the type of herniation, the anatomy, the team’s experience and the real objective of the procedure.
When will I be able to drive or work?
There is no universal date. It depends on pain, the type of job, the medication you take and your clinical progress. It is sensible to discuss ranges and adapt return to activity progressively.
Glossary
- Lumbar disc herniation: protrusion or displacement of part of the intervertebral disc in the lower back.
- Sciatica: pain that travels down the leg due to irritation or compression of a lumbar nerve root.
- Radiculopathy: a set of symptoms resulting from involvement of a nerve root, such as pain, tingling, loss of sensation or weakness.
- Microdiscectomy: surgery aimed at removing the disc fragment that compresses the nerve.
- Neurological deficit: loss of strength, sensation or reflexes due to nervous system involvement.
- Recurrence: reappearance of the problem after a previous improvement, for example a new herniation at the same level.
- Dura mater: the membrane that surrounds the nerve roots and cerebrospinal fluid.
- Cerebrospinal fluid leak: escape of the fluid that surrounds the nerves and spinal cord through an accidental opening of the dura mater.
In summary, lumbar microdiscectomy should not be seen either as a failure or as a magic solution. It is a useful tool when the problem is well defined, when the pain or deficit justifies it and when there is an honest understanding of what can improve, what risks exist and what the real recovery will be like.
References
- North American Spine Society – Lumbar Disc Herniation with Radiculopathy
- NICE – Low back pain and sciatica in over 16s: assessment and management
- ACR Appropriateness Criteria – Low Back Pain
- AANS – Herniated Disc
- A Systematic Review of Treatment Guidelines for Lumbar Disc Herniation
- Indications for surgery versus conservative treatment in the management of lumbar disc herniations
- Return to Work After Lumbar Microdiskectomy
- Discectomy versus sequestrectomy in the treatment of lumbar disc herniation
- Risk Factors and Reoperation Rate in Revision Lumbar Disc Herniation Surgery
- Patient Factors Associated with Recurrent Herniation and Revision Surgery Following Lumbar Microdiscectomy
- Management of recurrent lumbar disc herniation
- Full-endoscopic versus microscopic lumbar discectomy
This content is educational and does not replace an individual medical evaluation. The final decision depends on your symptoms, your examination, your imaging tests and your response to conservative treatment.