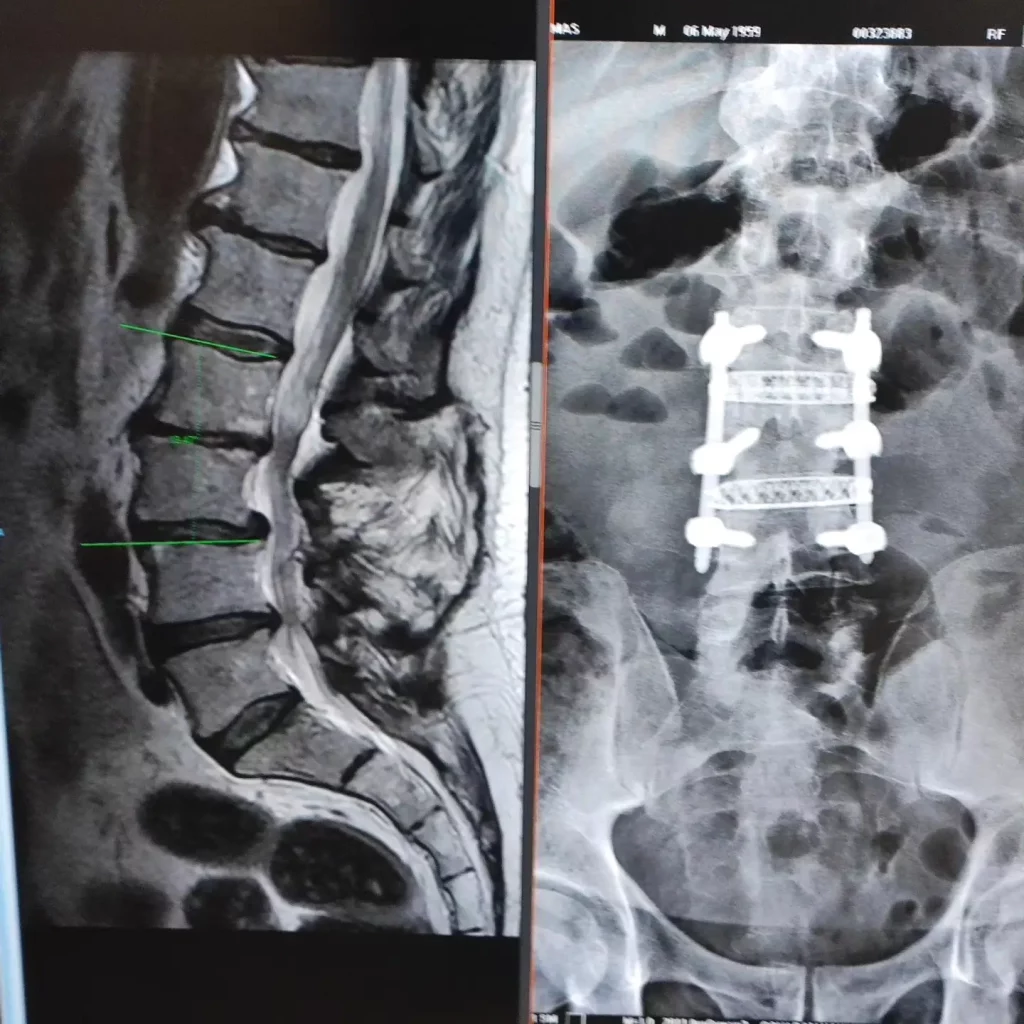
After a cervical or lumbar fusion, many people improve noticeably. But sometimes, months or years later, new pain appears, tingling returns, or walking becomes difficult again. It does not always mean the same thing. In some cases, the problem is in the segment adjacent to the previous surgery, and this is known as adjacent segment syndrome.
Adjacent segment syndrome is not simply “wear and tear for no reason” nor does it mean that every fusion ends badly. It refers to when the level above or below a fusion develops changes that also produce real symptoms, such as radicular pain, claudication, weakness or even spinal cord compression. The challenge is to distinguish it from other similar scenarios, such as pseudoarthrosis, recurrent disc herniation, sacroiliac pain or an expected postoperative evolution.
What adjacent segment syndrome is — and what it is not
First it is useful to clarify an important nuance. Seeing changes on an X-ray or MRI is not the same as having a symptomatic disease. Many operated patients develop some degeneration at the adjacent level over time and do not therefore need treatment. We talk about adjacent segment syndrome when those changes are associated with symptoms and real functional limitation.
It can occur in the cervical or lumbar spine. In the neck it usually presents with pain radiating to the arm, tingling, loss of strength or signs of spinal cord compression. In the lumbar spine the most typical findings are pain radiating to the leg, a heavy feeling when walking, new mechanical pain or progressive worsening of function.
The cause does not depend on a single factor. Biomechanics after fusion, age, the preoperative condition of adjacent discs, spinal alignment, bone quality, the number of levels operated and, in some cases, technical decisions in the initial procedure all play a role. That is why two people with similar surgery can have very different outcomes.
9 signs that may raise suspicion
1. You improved after surgery and months or years later a different pain appeared
One of the most common clues is having had a reasonably good period and then noticing a new pain. It does not have to be unbearable, but it is different from the usual recovery pain.
2. The pain moves down the arm or leg in a nerve pattern
If the pain travels down an arm or a leg, with tingling, electric sensations, numbness or loss of strength, consider radicular compression at the adjacent level.
3. Walking becomes difficult and sitting relieves you
In the lumbar area, when neurogenic claudication appears, many people report they can only walk a certain distance and need to stop or sit down to continue.
4. The neck or back again feels “stiff” but not only because of the prior fusion
5. Clumsiness in the hands, worse balance or an unsteady gait appears
This is especially important in the cervical spine. It may suggest myelopathy, that is, involvement of the spinal cord, and should not be trivialized.
6. The pain no longer fits the typical recovery timeline
After a fusion it is normal to have discomfort for weeks or months. The alarm sign is when the pattern changes, plateaus or clearly worsens without a simple explanation.
7. Posture worsens or it becomes harder to stay upright
In the lumbar spine, poor alignment or overload of adjacent levels can make standing for long periods increasingly difficult.
8. Previous tests “looked fine,” but function keeps declining
Sometimes an old MRI or a single X-ray does not fully explain what is happening. When function worsens, symptoms, clinical exam and updated imaging must be re-correlated.
9. You were told everything is “normal for the surgery” but the real impact is increasing
Not all late postoperative pain is normal. If it affects sleep, work, walking or basic tasks, the case should be reviewed in context and not dismissed with a reassuring phrase.
How it is reasonably diagnosed
The diagnosis should not be made based only on an MRI nor solely on what the patient feels. The key is to combine clinical history, neurological examination and imaging. The aim is to answer three questions: what symptoms are present, at which level they could originate, and whether that level is adjacent to the previous fusion.
Magnetic resonance imaging (MRI) is usually the most useful test when there is radiating pain, suspicion of stenosis, radiculopathy or spinal cord compression. Dynamic X-rays can help if instability is suspected. CT is especially useful when the previous fusion, the hardware or bony alignment need review.
It is also important not to fall into automatic diagnoses. A patient with pain after a fusion may have pseudoarthrosis, facet pain, sacroiliac pain, a recurrent hernia or even a non-spinal cause. The best diagnosis is usually the one that explains the clinical picture, the exam and the imaging together, not the one that sounds most spectacular.
Non-surgical alternatives
Not all cases end in a new operation. If there is no progressive neurological deficit or significant instability, it is often reasonable to start with conservative options. The goal is to reduce pain, recover function and gain time to observe the real evolution.
The most common measures include education, adapted activity, targeted physiotherapy, cautious analgesia and, in selected cases, injections or interventional techniques on facets or nerve roots. In some profiles, especially when the pain is mixed and there is no marked deformity or instability, this can be sufficient to control symptoms.
It is important to have realistic expectations. Conservative treatment does not “un-fuse” the spine nor correct severe compression, but it can greatly improve quality of life in moderate cases or help decide more calmly whether surgery is justified.
When surgery may be considered
Surgery usually enters the discussion when well-conducted conservative measures fail, when there is progressive neurological deficit, or when there is instability, deformity or relevant compression of roots or the spinal cord.
There is no single operation valid for everyone. Sometimes a focal decompression is enough if the main problem is nerve compression and the spine is stable. In other cases the fusion must be extended, alignment corrected or decompression combined with new instrumentation. In selected profiles, some motion-preserving techniques or minimally invasive approaches may be an option, but they depend heavily on the anatomical context and the previous surgery.
The important question is not “can I be operated on,” but “what specific objective does that surgery pursue.” Decompressing a root, stabilizing a segment, correcting a malalignment or addressing a mechanical failure are different scenarios, with different risks and recoveries.
Real benefits and risks of treatment
Expected benefits
When the indication is correct, the most reasonable benefits are relief of radicular pain, improved gait, reduced claudication, recovery of strength or halting neurological deterioration. In some cases functional posture and tolerance for standing also improve.
Risks and adverse effects
Conservative treatment may not be sufficient. Injections can relieve temporarily and do not always change the natural course. Surgery, on the other hand, can involve infection, bleeding, nerve injury, cerebrospinal fluid leak, thrombosis, hardware failure, nonunion and the possibility of needing further revisions.
Also, a reoperation does not mean a “fresh start.” It is usually more demanding than a primary surgery and requires especially careful planning. That said, this does not mean it is doomed to fail. It means the benefit-risk balance must be very clearly explained.
Referral criteria
Specialized evaluation should be requested if disabling radicular pain appears after a fusion, if walking becomes progressively more difficult, if there is progressive weakness, if persistent tingling returns, or if there is a clear change compared with the initial improvement.
Referral should be faster when there is suspicion of cervical myelopathy, signs of instability, severe pain with rapid functional deterioration, or reasonable doubts about whether the problem is the adjacent segment, the previous fusion or another pain source.
Realistic recovery times
There is no single timetable. If management is conservative, some improvement may be seen in 6 to 12 weeks, provided the plan is well directed. After a revision surgery or fusion extension, recovery depends on the level, whether only decompression or also instrumentation was performed, bone quality and overall health.
Very roughly, light tasks can be resumed in a few weeks after limited procedures. Return to sedentary work can take several weeks. If the surgery is more extensive or physically demanding, timelines can extend to months. The most honest approach is to discuss ranges rather than miracle dates.
When to go to the emergency room
There are symptoms that should not wait for a routine appointment. In the lumbar area, highlight urinary retention, new incontinence, saddle anesthesia and rapidly progressive leg weakness. In the cervical spine, especially worrisome signs are rapid loss of strength, worsening gait, marked hand clumsiness or signs of spinal cord compression.
Fever with intense pain, an inflamed surgical wound or pain accompanied by general deterioration also require urgent attention, because they force consideration of infection or other complications.
Myths and realities
Myth: if there is degeneration at the adjacent level, I will surely have symptoms
Reality: no. There are radiological findings that never become clinically relevant problems.
Myth: if my back or neck hurts again, the fusion “went wrong”
Reality: it can be due to several causes, including the adjacent segment, but also other mechanical or neurological sources.
Myth: a new operation will always be worse than the first
Reality: a revision can be more complex, but when it corrects the real cause it can bring significant improvement.
Myth: minimally invasive techniques work for every case
Reality: they help in well-selected profiles, but do not replace clinical judgment or the need to stabilize when necessary.
Frequently asked questions
Can it appear years after surgery?
Yes. It can appear months after, but also several years later. The exact timing varies widely between people.
Does it mean the first operation was a mistake?
Not necessarily. Sometimes it is part of biomechanical evolution and the preexisting condition of the spine, not an isolated technical error.
Does it always require another fusion?
No. It depends on whether there is instability, deformity, neurological compression and how you respond to conservative options.
Does the MRI confirm it by itself?
No. Imaging helps a lot, but it must be correlated with symptoms and the clinical exam.
Can I exercise if this is suspected?
In many cases yes, with adaptation and professional guidance. But if there is progressive weakness or signs of spinal cord or cauda equina compression, the priority is urgent assessment.
Can it be completely prevented?
Not always. Risks can be reduced with good surgical indication, reasonable alignment correction, maintained bone health and appropriate follow-up.
Does arthroplasty completely prevent this problem?
No completely. It can reduce some risks in selected profiles, but it is not an absolute guarantee and is not suitable for all patients.
Glossary
- Spinal fusion: surgery that joins two or more vertebrae to eliminate painful or unstable movement.
- Adjacent segment: the level immediately above or below a previous surgery.
- Radiculopathy: pain, tingling or weakness due to irritation of a nerve root.
- Myelopathy: involvement of the spinal cord, often with clumsiness, worse balance or weakness.
- Neurogenic claudication: pain or heaviness when walking due to nerve compression, which usually improves when sitting.
- Pseudoarthrosis: lack of bone consolidation after a fusion.
- Decompression: surgery aimed at giving more space to nerves or the spinal cord.
References
- Complex Spine Institute. Extreme lateral interbody fusion (XLIF).
See reference - Complex Spine Institute. Oblique lateral interbody fusion (OLIF).
See reference - Huang X et al. Risk factors and treatment strategies for adjacent segment disease following spinal fusion. 2024.
See reference - Zhu Q et al. Incidence of Adjacent Segment Degeneration and Its Associated Risk Factors Following ACDF: A Meta-Analysis. 2024.
See reference - Wang N et al. Safety and clinical efficacy of endoscopic procedures for the treatment of adjacent segmental disease after lumbar fusion. 2023.
See reference - Zavras AG et al. Effect of device constraint: a comparative network meta-analysis of ACDF and cervical disc arthroplasty. 2024.
See reference - American Association of Neurological Surgeons. Cauda Equina Syndrome.
See reference - American College of Radiology. Appropriateness Criteria: Low Back Pain, with a specific section for suspected cauda equina and a history of lumbar surgery with new or progressive symptoms.
See reference - NICE CKS. Neck pain – cervical radiculopathy: management, with recommendation for urgent referral in the presence of red flags.
See reference
This content is for educational purposes and does not replace an individual medical assessment. If you have progressive neurological symptoms, changes in sphincter control, fever or rapid worsening, seek urgent medical attention.